Are you suffering from varicose veins or concerned you might be at risk for developing them? In this complete guide, physician, Dr. G. Ian Shore discusses and explains everything you need to know about varicose vein disease. From understanding the risk factors to being able to identify the subtle symptoms, and finally, understanding the latest office-based treatments for chronic venous disease, this article will hopefully answer all questions and encourage anyone thinking they may have symptoms related to chronic venous disease to go and get a free vein screening at an accredited vein center.
With no “down” time and very minimal discomfort, treatment is easy and available to all ages, regardless of other medical conditions. Also, it is important to emphasize that all treatments are office-based procedures, thus having now eliminated any hospital interventions as compared to in the past. This review should help you recognize if you might be suffering from chronic vein disease and how easy it is to be evaluated and treated by an expert vein specialist with the assistance of ultrasound imaging right in the office. A primary care referral is usually unnecessary; office evaluations take 30 minutes or less. Normal activities can be resumed the next day!
Even more importantly, almost all medical insurances cover office-based therapeutic options. Dr. G. Ian Shore also offers insights into the different treatments, possible complications associated with each one, and the best preventive methods. Whether you’re looking for information or seeking answers, this guide is your go-to resource.
What are Varicose Veins?
Varicose veins are stretched and/or twisted veins with abnormally elevated pressure associated with reflux that usually appear in the legs over time. Without treatment, continued damage to the valves within the vein walls will occur, leading to the veins’ deteriorating function and further problems. Unfortunately, this process had usually been ongoing for many years before affected individuals sought medical intervention, only because now there has been the development of visual changes in the legs from this ongoing chronic venous disease that alerts them to the problem. Often, significant decreases in the quality of life of many affected individuals are already present at the time of diagnosis. Early symptom recognition of chronic venous disease of the legs is critical, allowing proactive intervention that can prevent progression to significant complications.
The damaged refluxing veins are generally located just below the skin, can appear blue or purple and can be seen quite easily in cases when longstanding reflux disease has been ongoing untreated for many years. These visible “bulging” veins will be seen in some patients, that are not only visibly unpleasant but can also bleed when traumatized and cause other annoying symptoms. In the earlier phases of refluxing blood flow in these damaged veins, visual signs are often not present; however, ongoing damage occurs, usually associated with only very subtle symptoms (like night cramps and restless legs).
The valves in veins are responsible for assuring blood courses in one direction against gravity, towards the heart. When these valves become damaged, blood begins to flow in the opposite direction, towards the feet and ankles, thus causing blood to pool in the veins of the legs, causing them to stretch and leak, and can cause daily ankle swelling. Consequently, somebody with varicose veins may also experience discomfort, swelling, cramping, burning, and a feeling of heaviness in their legs, especially at the end of the day, especially after prolonged sitting or standing. Many times, these symptoms are wrongly confused with other conditions like neuropathy and arthritis, which are much less common than chronic venous disease. It is estimated that 50% of the adult population in this country suffers from various stages of chronic vein disease of the legs.
This is in stark contrast to only up to 10% of the general adult population that suffers from peripheral neuropathy. Chronic venous disease of the legs is vastly underdiagnosed and is becoming a huge health problem. Sadly, if diagnosed early, many of the long-term consequences can be avoided with office-based treatments with no downtime and almost no pain, and improved quality of life.
What Causes Varicose Veins?
The causes of varicose veins are mainly related to damage to the valves in the veins, resulting in a disturbance in the proper blood flow within the venous system of the legs. Once the veins are damaged, they cannot be fixed.
When the valves in the veins malfunction, they fail to prevent the backflow of blood against gravity, causing it to pool in the legs and exert excessive high pressure, thus causing “leakage” of blood through the thin and stretched vein wall. This weakening of the walls of the veins eventually leads to progressive leakage of fluid into the surrounding tissue, with resultant chronic swelling and fluid “weeping” from the skin. If not treated sooner, this could lead to infection and ulceration. Consequently, insufficient arterial circulation can also occur, restricting the appropriate allowance of nutrients and oxygen to the surrounding tissues and skin. The skin can also become stained with a brownish discoloration, thickened, and dry, especially in the shin area. Sometimes, venous ulceration of the skin in the medial lower leg can occur, which is very difficult to treat.
Who is at Risk for Varicose Veins?
People with a family history of varicose veins, those who stand or sit for long periods, obesity, smoking, and individuals with other specific medical conditions, like diabetes, are at a more increased risk of developing this chronic disease and its complications.
Genetics plays a significant role in the susceptibility of developing varicose veins. If your parents or siblings have varicose veins, you are also more likely to develop them. Lifestyle changes such as limiting standing or sitting for prolonged periods, exercising regularly, and maintaining proper weight can help reduce the susceptibility to this vein problem.
How are Varicose Veins Diagnosed?
Diagnosing varicose veins typically requires a thorough examination of the affected areas, including medical history and physical examination by a healthcare provider.
During the medical record check, the healthcare provider will ask if any family member had varicose veins, previous therapies, and any underlying medical disorders that may contribute to vein problems. The physical assessment may include a visual examination of the veins, palpation to consider the size and texture of the veins with associated pitting edema, and inspection for any signs or symptoms of chronic skin changes like brown staining and healed previous skin ulcer scars.
What are the Symptoms of Varicose Veins?
Common symptoms of varicose veins include enlarged burning veins, achiness, and/or heaviness in the legs, with skin color changes near the affected veins.
Some people with varicose veins may also experience itchiness, throbbing, or cramping in the areas. Night cramps and restless leg syndrome are common symptoms suggesting underlying chronic venous disease. People may also notice dryness or thickening of the skin on the anterior shin area.
What are the Methods of Diagnosis?
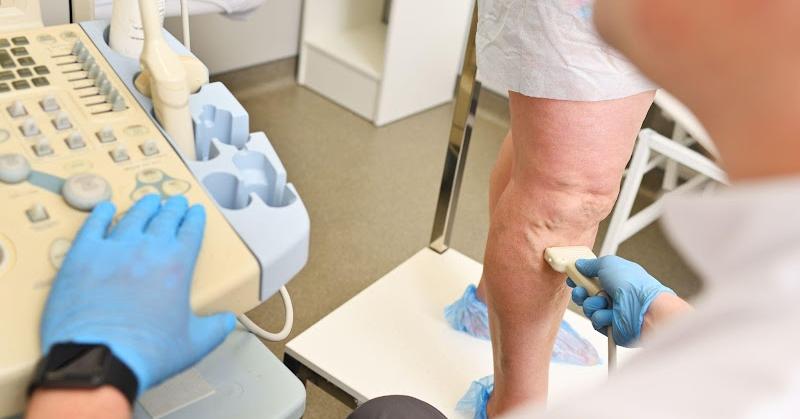
Analyzing for the presence of varicose veins always involves imaging examinations such as ultrasound Doppler scans. This is performed in the office by a highly trained vascular ultrasound technician to visualize the extent and severity of the vein disease and evaluate for abnormal blood flow direction (reflux). Also, home compression stocking trials can be used for several weeks to help confirm the diagnosis in equivocal findings on ultrasound.
These imaging techniques are vital in identifying all the diseased veins and their locations. (creating a road map for treatment ). Ultrasound imaging also allows healthcare specialists to look for any other expected oddities. The team of venous experts can then create a comprehensive strategy for treatment of the patient’s overall venous disease and formulate a personalized treatment plan that is best suited for that patient’s varicose vein disease.
What are the Treatment Options for Varicose Veins?
Treating varicose veins involves a spectrum of options, including lifestyle modifications, removal treatment, laser treatment, and medicine tailored to the person’s circumstances and preferences.
Lifestyle Changes
Lifestyle changes such as standard training, maintaining a healthy diet, weight control, and avoiding prolonged sitting or standing can control symptoms of varicose veins.
Interspersing routines into daily habits, such as walking, swimming, or cycling, can enhance circulation and reduce the inflation in your veins. A diet rich in fruits and vegetables can help with general vascular fitness.
Compression Therapy
Compression therapy, often using specially fitted compression socks, assists in improving blood flow in the legs, decreasing swelling and discomfort associated with varicose veins. Although not a permanent treatment modality, compression is valuable after thermal and chemical treatments to help improve success and recovery.
These compression socks work by exerting gentle pressure on the legs, helping the veins push blood back toward the heart. By enhancing circulation and controlling blood from pooling in the veins, compression therapy can significantly help reduce symptoms such as swelling, achiness, and cramping, but does not “fix” the problem. Wearing these socks can decrease the symptoms related to varicose veins, however once removed, the symptoms will quickly return.
Laser/RFA Therapy(thermal)
Laser or radiofrequency therapy for varicose veins involves using concentrated light/electric energy to target and permanently seal off damaged truncal veins, a 45-minute office-based procedure with minimal pain and almost immediate recovery times.
This treatment option is highly accurate in targeting only the large refluxing truncal veins while minimizing injury to surrounding tissues and nerves, resulting in less pain for patients. By utilizing the laser’s heat to “close off” the more prominent refluxing veins, blood flow is then re-circulated to healthier undamaged veins, therefore eliminating chronic symptoms like bulging, heaviness, and cramping discomfort. Patients also enjoy a shorter recovery period with laser or radiofrequency treatment, allowing them to return to normal activities sooner than had been possible with conventional surgery techniques of the past.
Ultrasound-Guided Foam Therapy(chemical)
Ultrasound-guided foam therapy (also known as ultrasound-guided sclerotherapy with foam) is a relatively fast, safe, and minimally invasive method for treating varicose veins and achieving lasting results.
Injected directly into the veins under the guidance of ultrasound technology, foam sclerosant quickly displaces the blood, reducing the vein’s size by complete spasm and then causing it to permanently scar, resulting in the vein’s eventual reabsorption into the body. This is the newest and most efficient option for both acute and chronic treatment of chronic venous insufficiency. .
Foam therapy for varicose veins leaves no scarring, has minimal risk of side effects and is proven to deliver results quickly.
Complications
As with any procedure, complications and expectations need to be explained. Discomfort for 48-72 hours after treatment is expected, as well as some redness overlying the treated veins. These are not complications.
Some pigmentation at the injection site may also occur but usually resolves within 3-4 months.
DVT can occur but is very uncommon. It has been reported as low as 0.07% in large series. The majority of cases rarely require any treatment besides close observation.
Infection and bleeding are also very rare.
Long Term Expectation
Once all required vein treatment sessions have been completed, patients will be explained the importance of coming yearly for an ultrasound re-evaluation of the legs, for any new refluxing veins, even if they are having no new symptoms. Also, compression stockings are always recommended for long(greater than 2 hours) car trips or airline flights to help slow down the recurrence of varicose veins and venous insufficiency.
Note: varicose veins are a chronic disease. Patients will require lifelong follow-up with their physician to ensure any new malfunctioning veins are identified and treated promptly.